Liposuction
| Liposuction | |
|---|---|
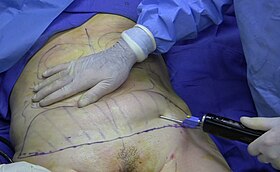 A plastic surgeon performing liposuction surgery | |
| Other names | Lipoplasty, lipectomy, fat modeling, liposculpture, suction lipectomy, suction-assisted fat removal, lipo, lymph-sparing liposuction, tumescent liposuction, water-assisted liposuction, power-assisted liposuction, laser-assisted liposuction, ultra-sound assisted liposuction |
| ICD-10-PCS | 0JDL3ZZ: RT UPPER LEG; 0JDM3ZZ: LT UPPER LEG; OJDN3ZZ: RT LOWER LEG; 0JDP3ZZ: LT LOWER LEG |
| MeSH | DO65134 |
| MedlinePlus | 002985 |
| Part of a series on |
| Human body weight |
|---|
Liposuction, or simply lipo, is a type of fat-removal procedure used in plastic surgery.[1] Evidence does not support an effect on weight beyond a couple of months and does not appear to affect obesity-related problems.[2][3] In the United States, liposuction is the most common cosmetic surgery.[4][5]
The procedure may be performed under general, regional, or local anesthesia. It involves using a cannula and negative pressure to suck out fat.[4] As a cosmetic procedure it is believed to work best on people with a normal weight and good skin elasticity.[4]
While the suctioned fat cells are permanently gone, after a few months overall body fat generally returns to the same level as before treatment.[2] This is despite maintaining the previous diet and exercise regimen. While the fat returns somewhat to the treated area, most of the increased fat occurs in the abdominal area. Visceral fat—the fat surrounding the internal organs—increases, and this condition has been linked to life-shortening diseases such as diabetes, stroke, and heart attack.[2]
Cosmetic liposuction[]
There are two different uses for liposuction: cosmetic liposuction to change the body's contour or shape and reconstructive, medically necessary liposuction. Reconstructive uses include treatment of lipedema,[6] to remove excess fat in the chronic medical condition lymphedema,[7] and to remove lipomas from areas of the body.[8][9]
Cosmetic liposuction should not be used as a weight-loss plan but to aesthetically improve the appearance of body parts and contour.[10] Benefits from cosmetic liposuction appears to be of a short term nature with little long term effect.[2] After a few months fat typically returns and redistributes.[2] Liposuction does not help obesity related metabolic disorders like insulin resistance.[3]
Reconstructive, medically necessary liposuction[]
The neutrality of this section is disputed. (August 2021) |
There are many articles and references to liposuction as "cosmetic" and not reimbursed by medical insurance companies. Most of this information is outdated. If the documentation supports the liposuction for a medical reason (lipedema, lymphedema, lipomas) as reconstructive, and not investigational, experimental, or unproven, the claim is medically necessary and should be reimbursed.[11] While most insurance companies may initially deny the claim, many can be won upon appeal if the documentation and patient's need supports the criteria for reconstructive surgery.[12][13][14]
The techniques and terms listed below: tumescent, lymph-sparing, Tumescent Local Anesthesia (TLA), Water-Assisted Liposuction (WAL), Power-Assisted Liposuction (PAL), Laser-Assisted Liposuction (LAL) all apply to reconstructive, medically necessary liposuction.[15][16]
Techniques[]

In general, fat is removed via a cannula (a hollow tube) and aspirator (a suction device). Liposuction techniques can be categorized by the amount of fluid injected, and by the mechanism by which the cannula works. If the removed fat is used as filler for the face, lips, or breasts knowledge of the precise technique used to remove the fat is indicated.[17]
There are numerous types of liposuction. Some can be described as techniques or modalities. Often surgeons will use two or more of the different techniques below in the same session.
Suction-assisted liposuction (SAL)[]
This is the most generic term for liposuction. In the CPT manual it is referred to as "suction-assisted lipectomy" and includes codes: 15876-15879.[18]
Micro-cannula[]
This does not address a particular technique but the diameter of the cannula, a stainless steel tube which is inserted into subcutaneous fat through a small opening or incision in the skin. The outside diameter of micro-cannulas range from 1 mm to 3 mm.[19]
Lymph-sparing liposuction[]
This technique does not require a particular wand and is most often performed with either tumescent liposuction or WAL (below). It refers to the specific surgical technique, the skill of the surgeon, and the extensive training that is unique to removing lipedema fat.[20] Because the scope is different for removal of lipedema fat versus cosmetic contouring, if lymph-sparing is not addressed in the surgical operative notes, a medical necessity review committee could determine that the procedure poses “a risk to the lymph system.”[21][22][23]
Tumescent local anesthesia (TLA)/tumescent liposuction[]
This may be referenced either way above, but the technique is the same.[24] This is an anesthesia technique recommended for lymph-sparing liposuction surgery. Tumescent Liposuction refers to the use of anesthesia during liposuction. The word “tumescent” means swollen and firm. By injecting a large volume of very dilute lidocaine (local anesthetic) and epinephrine (capillary constrictor) into subcutaneous fat, the targeted tissue becomes swollen and firm, or tumescent. This technique does not require a special or specific type of wand.[19][20]
Power-assisted liposuction (PAL)[]
Referred to as "a vibrating cannula" in research studies, PAL uses a specific type of wand that creates an up and down, vibrating-like motion of the cannula to acquire greater fat removal. When compared to simple suction-assisted liposuction, PAL requires less energy for the surgeon to operate while also resulting in greater fat removal. It is commonly used for difficult, secondary, scarred areas, and when harvesting large volumes of fat for transfers to other areas.[25][26]
Note that techniques can be combined; for instance one could refer to the procedure as "lymph-sparing, tumescent liposuction using a vibrating (PAL) microcannula to treat lipedema."
Water-jet assisted liposuction (WAL)[]
A specific technique and wand commonly used for patients who require lymph-sparing liposuction for lipedema. The lipedema fat is removed using a fan-shaped jet of water, which includes the anesthetic. In contrast to tumescent liposuction above, where the anesthetic solution is injected separately and beforehand, the WAL wand both injects the solution and suctions the fat. BodyJet is a Water-Assisted Liposuction system.[27]
Fibro-lympho-lipo-aspiration (FLLA)[]
This rare and unique term for liposuction for lipedema is used in a specific paper by Campisi, Fibro-Lipo-Lymph-Aspiration With a Lymph Vessel Sparing Procedure to Treat Advanced Lymphedema After Multiple Lymphatic-Venous Anastomoses: The Complete Treatment Protocol. This term emphasizes the uniqueness of the reconstructive procedure versus the cosmetic procedure. Everything about the surgical suction application via cannula is different from standard suction lipectomy. The goal of FLLA is to relieve symptoms such as pain, ameliorate disability, improve function and quality of life, and halt disease progression.
Only small blunt cannulas are used, great care is used to not injure lymphatic which are already abnormal and increased risk of injury. Only the longitudinal orientation of cannulas is used at critical junctures. Preoperatively critical lymphatic structures are scanned and marked. FLLA surgery is significantly more time-consuming than cosmetic surgery often requiring 4–5 hours per body part; much larger aspirate volume is removed versus cosmetic suction lipectomy.
The benefit to lymphatics function comes not only from the removal of subcutaneous adipose tissue, but also the all components of the loose connective tissue including removing fibrosis in the interstitial space.[28]
Ultrasound-assisted liposuction (UAL)[]
Ultrasound-assisted liposuction techniques used in the 1980s and 1990s were associated with cases of tissue damage, usually from excessive exposure to ultrasound energy.[29] Third-generation UAL devices address this problem by using pulsed energy delivery and a specialized probe that allows physicians to safely remove excess fat.[30] UAL is beneficial in people with a particular skin tone, in liposuction of areas that are more difficult to remove fat, that include treatment of gynecomastia, or areas where secondary liposuction is being performed.[31]
Laser-assisted liposuction/lipolysis (LAL)[]
Referred to as Smart Lipo, this technique uses laser technology to coagulate and tighten the skin and boost collagen performance.[32] Uses include "cankles", debulking surgery for elephantiasis nostras [33] and lipedema.[34]
Cryolipolyis or fat freezing[]
Sold under the brand name of CoolSculpting, cryolipolyis is not a type of liposuction but rather a non-surgical fat reduction procedure that freezes fat cells; it is an FDA-approved, non-invasive procedure that uses the power of cooling to disrupt fat cells underneath the dermis.[35] This freezing energy crystallizes and eventually kills targeted fat cells without harming the surrounding healthy tissue. The body's metabolic processes work to remove the dead fat cells.[36][37] Coolsculpting is not recommended for those with lipedema, lymphedema or other conditions that affect the lymphatic system.
After care—sutures[]
Doctors disagree on the issues of scarring with not suturing versus resolution of the swelling allowed by leaving the wounds open to drain fluid. Suturing is more common with a large cannula.[26] Since the incisions are small, and the amount of fluid that must drain out is large, some surgeons opt to leave the incisions open, while others suture them only partially, leaving space for the fluid to drain out.[38]
Safety and risks[]
Liposuction is considered very safe, however not all liposuction surgery is equal. Small volume liposuction (<1000 cc) done awake is different from large volume liposuction (>5000 cc, in some cases 10,000 cc) done with anesthesia and a hospital stay.[39]
Suction-assisted lipectomy (aka liposuction) were identified from the Tracking Operations and Outcomes for Plastic Surgeons database maintained by The American Society of Plastic Surgeons (ASPS).[40] The ASPS maintains a registry of plastic surgery cases called TOPS (Tracking Operations & Outcomes for Plastic Surgeons) which is the largest database of plastic surgery cases.
Based on this database, no deaths were found in about 4,500 cases done by plastic surgeons. However, non-plastic surgeons are not included in this.[41]
In the (Chow I., et al., 2015) study, sixty-nine of 4534 patients (1.5 percent) meeting inclusion criteria experienced a postoperative complication. Their conclusion was that: Liposuction by board-certified plastic surgeons is safe, with a low risk of life-threatening complications. Traditional liposuction volume thresholds do not accurately convey individualized risk. The authors' risk assessment model demonstrates that volumes in excess of 100 ml per unit of body mass index confer an increased risk of complications.[42]
There exists a spectrum of complications that may occur due to any liposuction. Risk is increased when treated areas cover a greater percentage of the body, incisions are numerous, a large amount of tissue is removed, and concurrent surgeries are done at the same time. To address safety issues, the American Society of Plastic Surgeons (ASPS) published in 2009 Evidence-Based Patient Safety Advisory: Liposuction
This 17-page document addresses key safety issues and offers recommendations.[40] In addition, the increase in tumescent and lymph-sparing techniques have had a positive impact on diminishing complications.[43] In a 2009 paper, the author found from a series of 3,240 procedures, no deaths occurred, and no complications requiring hospitalization were experienced. In nine cases, complications developed that needed further action. The conclusion was that liposuction using exclusively Tumescent Local Anesthesia (TLA) is a proven safe procedure provided that the existing guidelines are meticulously followed.[44][20]
Some side effects and complications include, but are not limited to, the following:
- Pain, which may be temporary or chronic
- Post-liposuction fat redistribution or post liposuction weight gain
- Bruising
- Infections
- Embolisms may occur when loosened fat enters the blood through blood vessels ruptured during liposuction. Pieces of fat can wind up in the lungs, or even the brain. Fat emboli may cause permanent disability or, in some cases, be fatal.
- Puncture wounds in the organs (visceral perforations) may require surgery for repair. They can also prove fatal.
- Seroma is a pooling of serum, the straw-colored liquid from blood, in areas where tissue has been removed.[45]
- Paresthesias (changes in sensation that may be caused by nerve compression) is an altered sensation at the site of the liposuction. This may either be in the form of an increased sensitivity (pain), or numbness in the area. In some cases, these changes in sensation may be permanent, although typical patients recover over the span of several weeks.[45]
- Swelling, in some cases, may persist for weeks or months after liposuction.
- Skin necrosis occurs when the skin above the liposuction site changes color and falls off. Large areas of skin necrosis may become infected with bacteria or microorganisms.
- Burns can occur during ultrasound-assisted liposuction if the ultrasound probe becomes hot.
- Fluid imbalance may impact you after you go home. The condition can result in serious ailments such as heart problems, excess fluid collecting in the lungs, or kidney problems.
- Toxicity from anesthesia due to the use of lidocaine, a skin-numbing drug, can cause lightheadedness, restlessness, drowsiness, a ringing in the ears, slurred speech, a metallic taste in the mouth, numbness of the lips and tongue, shivering, muscle twitching and convulsions. Lidocaine usage has already been linked to deaths from liposuction.[46]
- Scars at the site of the incision are usually small and fade with time, although some may be larger or more prominent.
- Deformities in the shape of the body may occur at the liposuction site after the procedure for about 20% of patients.[45]
- Death
Serious complications include deep vein thrombosis, organ perforation, bleeding, and infection.[47] Death occurs in about one per ten thousand cases.[48]
History[]
In 1977, Fischer and Fischer reviewed 245 cases with the planotome instrument for treating cellulite in the lateral trochanteric (hip-thigh) areas. There was a 4.9 per cent incidence of seromas, despite incision-wound suction catheters and compression dressings; 2.0 per cent of the cases presented pseudo-cyst formation that required removal of the capsule (cyst) through a wider incision (+ 5.0 mm) and the use of the panotome.[49][50]
Relatively modern techniques for body contouring and removal of fat were first performed by a French surgeon, Charles Dujarier, but a 1926 case that resulted in the amputation of the leg of a French dancer due to excessive tissue removal and too-tight suturing set back interest in body contouring for decades.[51][52]
Liposuction evolved from work in the late 1960s from surgeons in Europe using techniques to cut away fat, which were limited to regions without many blood vessels due to the amount of bleeding the technique caused.[51] In the mid-1970s in Rome, Arpad and Giorgio Fischer created the technique of using a blunt cannula linked to suction; they used it only to remove fat on the outer thighs.[53] Yves-Gérard Illouz and Fournier extended the Fischers' work to the whole body, which they were able to use by using different sized cannulae.[51] Illouz later developed the "wet" technique in which the fat tissue was injected with saline and hyaluronidase, which helped dissolve tissue holding the fat, prior to suctioning.[51] Lidocaine was also added as a local anesthetic.[51] Fournier also advocated using compression after the operation, and travelled and lectured to spread the technique.[51] The Europeans had performed the procedures under general anesthesia; in the 1980s American dermatologists pioneered techniques allowing only local anesthetics to be used.[51] Jeffrey Klein published a method that became known as "tumescent" in which a large volume of very dilute lidocaine, along with epinephrine to help control bleeding via vasoconstriction, and sodium bicarbonate as a buffering agent.[51]
In 2015 liposuction surpassed breast augmentation surgery as the most commonly performed cosmetic procedure in the US.[54]
See also[]
- Bariatrics – branch of medicine that deals with the causes, prevention, and treatment of obesity
- Gastric bypass surgery
- Lipotomy
- Spot reduction
References[]
- ^ Dixit, VV; Wagh, MS (May 2013). "Unfavourable outcomes of liposuction and their management". Indian Journal of Plastic Surgery. 46 (2): 377–92. doi:10.4103/0970-0358.118617. PMC 3901919. PMID 24501474.
- ^ Jump up to: a b c d e Seretis, Konstantinos; Goulis, Dimitrios G; Koliakos, Georgios; Demiri, Efterpi (2015). "Short- and Long-Term Effects of Abdominal Lipectomy on Weight and Fat Mass in Females: A Systematic Review". Obesity Surgery. 25 (10): 1950–8. doi:10.1007/s11695-015-1797-1. PMID 26210190.
- ^ Jump up to: a b Seretis, K; Goulis, DG; Koliakos, G; Demiri, E (December 2015). "The effects of abdominal lipectomy in metabolic syndrome components and insulin sensitivity in females: A systematic review and meta-analysis". Metabolism: Clinical and Experimental. 64 (12): 1640–9. doi:10.1016/j.metabol.2015.09.015. PMID 26475176.
- ^ Jump up to: a b c Norton, Jeffrey A. (2012). Surgery Basic Science and Clinical Evidence. Berlin, Heidelberg: Springer Berlin Heidelberg. p. 2014. ISBN 9783642572821.
- ^ Khan, MH (November 2012). "Update on liposuction: clinical pearls". Cutis. 90 (5): 259–65. PMID 23270199.
- ^ Baumgartner A, Hueppe M, Schmeller W. Long-term benefit of liposuction in patients with lipoedema: a follow-up study after an average of 4 and 8 years. Br J Dermatol. 2016;174(5):1061-1067. doi:10.1111/bjd.14289
- ^ "Lymphoedema treatment". NHS Choices. NHS GOV.UK. July 18, 2017. Retrieved February 24, 2018.
- ^ https://www.uhcprovider.com/content/dam/provider/docs/public/policies/medadv-guidelines/c/cosmetic-reconstructive-services-procedures.pdf
- ^ Charifa A, Badri T. Lipomas, Pathology. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2020.
- ^ Davis W, Lawrence N. Weight Loss: How Does It Fit in With Liposuction? [published online ahead of print, 2019 Oct 24]. Dermatol Surg. 2019;10.1097/DSS.0000000000002225. doi:10.1097/DSS.0000000000002225
- ^ https://www.anthem.com/dam/medpolicies/abc/active/policies/mp_pw_a050277.html
- ^ https://www.cms.gov/medicare-coverage-database/details/lcd-details.aspx?LCDId=34698&ContrId=268&ver=28&ContrVer=1&CntrctrSelected=268*1&Cntrctr=268&s=5&DocType=1&bc=AAAAAAIAAAAA&
- ^ https://downloads.cms.gov/medicare-coverage-database/lcd_attachments/34698_20/L34698_GSURG032_BCG.pdf
- ^ https://www.novitas-solutions.com/webcenter/portal/MedicareJL/pagebyid?contentId=00099545
- ^ http://www.intechopen.com/books/advanced-techniques-in-liposuction-and-fat-transfer
- ^ Rubio, Alethia. (2015). Liposuction: Where are we and were are we going?. Anaplastology.
- ^ https://www.plasticsurgery.org/cosmetic-procedures/fat-transfer-breast-augmentation#
- ^ AMA CPT Manual 2020 Edition
- ^ Jump up to: a b Wollina, Uwe & Goldman, Alberto & Heinig, Birgit. (2010). Microcannular tumescent liposuction in advanced lipedema and Dercum's disease. Giornale italiano di dermatologia e venereologia : organo ufficiale, Società italiana di dermatologia e sifilografia. 145. 151-9.
- ^ Jump up to: a b c van de Pas, C. B., Boonen, R. S., Stevens, S., Willemsen, S., Valkema, R., & Neumann, M. (2020). Does tumescent liposuction damage the lymph vessels in lipoedema patients? Phlebology, 35(4), 231–236. https://doi.org/10.1177/0268355519885217
- ^ Leopoldo Cobos, MD, Karen Herbst, PhD, MD, Christopher Ussery, MS, CSCS, MON-116 Liposuction for Lipedema (Persistent Fat) in the US Improves Quality of Life, Journal of the Endocrine Society, Volume 3, Issue Supplement_1, April–May 2019, MON–116,
- ^ Sandhofer M, Hanke CW, Habbema L, et al. Prevention of Progression of Lipedema With Liposuction Using Tumescent Local Anesthesia: Results of an International Consensus Conference. Dermatol Surg. 2020;46(2):220‐228. doi:10.1097/DSS.0000000000002019
- ^ Lliposuccion
- ^ Schmeller W, Meier-Vollrath I. Tumescent liposuction: a new and successful therapy for lipedema. J Cutan Med Surg. 2006;10(1):7-10. doi:10.1007/7140.2006.00006
- ^ Tabbal, Geo N.; Ahmad, Jamil; Lista, Frank; Rohrich, Rod J. (November 2013). "Advances in Liposuction". Plastic and Reconstructive Surgery Global Open. 1 (8): e75. doi:10.1097/GOX.0000000000000007. ISSN 2169-7574. PMC 4186292. PMID 25289270.
- ^ Jump up to: a b Venkataram J. Tumescent liposuction: a review. J Cutan Aesthet Surg. 2008;1(2):49-57. doi:10.4103/0974-2077.44159
- ^ Stutz JJ, Krahl D. Water jet-assisted liposuction for patients with lipoedema: histologic and immunohistologic analysis of the aspirates of 30 lipoedema patients. Aesthetic Plast Surg. 2009;33(2):153-162. doi:10.1007/s00266-008-9214-y
- ^ Campisi CC, Ryan M, Boccardo F, Campisi C. Fibro-Lipo-Lymph-Aspiration With a Lymph Vessel Sparing Procedure to Treat Advanced Lymphedema After Multiple Lymphatic-Venous Anastomoses: The Complete Treatment Protocol. Ann Plast Surg. 2017;78(2):184-190. doi: 110.1097/SAP.0000000000000853.
- ^ Jewell, M (2008). "Innovation in Plastic and Aesthetic Surgery Lipoplasty". Innovations in Plastic and Aesthetic Surgery. pp. 443–53. doi:10.1007/978-3-540-46326-9_55. ISBN 978-3-540-46321-4.
- ^ De Souza Pinto, Ewaldo Bolivar; Chiarello De Souza Pinto Abdala, Priscila; Montecinos Maciel, Christovam; De Paula Turchiari Dos Santos, Fabiana; Pessoa Martello De Souza, Rodrigo (2006). "Liposuction and VASER". Clinics in Plastic Surgery. 33 (1): 107–15, vii. doi:10.1016/j.cps.2005.09.001. PMID 16427979.
- ^ Tabbal, Geo N.; Ahmad, Jamil; Lista, Frank; Rohrich, Rod J. (November 2013). "Advances in Liposuction". Plastic and Reconstructive Surgery Global Open. 1 (8): e75. doi:10.1097/GOX.0000000000000007. ISSN 2169-7574. PMC 4186292. PMID 25289270.
- ^ Leclère FM, Moreno-Moraga J, Mordon S, et al. Laser-assisted lipolysis for cankle remodelling: a prospective study in 30 patients. Lasers Med Sci. 2014;29(1):131-136. doi:10.1007/s10103-013-1279-4
- ^ Wollina U, Heinig B, Schönlebe J, Nowak A. Debulking surgery for elephantiasis nostras with large ectatic podoplanin-negative lymphatic vessels in patients with lipo-lymphedema. Eplasty. 2014;14:e11. Published 2014 Feb 28.
- ^ Wollina U, Heinig B, Nowak A. Treatment of elderly patients with advanced lipedema: a combination of laser-assisted liposuction, medial thigh lift, and lower partial abdominoplasty. Clin Cosmet Investig Dermatol. 2014;7:35-42. Published 2014 Jan 23. doi:10.2147/CCID.S56655
- ^ Ingargiola MJ, Motakef S, Chung MT, Vasconez HC, Sasaki GH.Plast Reconstr Surg. 2015 Jun;135(6):1581-90. doi: 10.1097/PRS.0000000000001236.PMID 26017594
- ^ Lipner SR.J Cosmet Dermatol. 2018 Apr;17(2):145-151. doi: 10.1111/jocd.12495. Epub 2018 Jan 17.PMID 29345049 Review.
- ^ Kilmer SL, Burns AJ, Zelickson BD.Lasers Surg Med. 2016 Jan;48(1):3-13. doi: 10.1002/lsm.22440. Epub 2015 Nov 26.PMID 26607045
- ^ MedlinePlus Medical Encyclopedia: Liposuction
- ^ Haeck, Phillip C. M.D.; Swanson, Jennifer A. B.S., M.Ed.; Gutowski, Karol A. M.D.; Basu, C Bob M.D., M.P.H.; Wandel, Amy G. M.D.; Damitz, Lynn A. M.D.; Reisman, Neal R. M.D., J.D.; Baker, Stephen B. M.D., D.D.S. the ASPS Patient Safety CommitteeAuthor Information
- ^ Jump up to: a b https://www.plasticsurgery.org/for-medical-professionals/advocacy/key-issues/liposuction
- ^ Haeck, Phillip C. M.D.; Swanson, Jennifer A. B.S., M.Ed.; Gutowski, Karol A. M.D.; Basu, C Bob M.D., M.P.H.; Wandel, Amy G. M.D.; Damitz, Lynn A. M.D.; Reisman, Neal R. M.D., J.D.; Baker, Stephen B. M.D., D.D.S. the ASPS Patient Safety Committee Evidence-Based Patient Safety Advisory: Liposuction, Plastic and Reconstructive Surgery: October 2009 - Volume 124 - Issue 4S - p 28S-44S doi: 10.1097/PRS.0b013e3181b52fcd
- ^ Chow I, Alghoul MS, Khavanin N, et al. Is There a Safe Lipoaspirate Volume? A Risk Assessment Model of Liposuction Volume as a Function of Body Mass Index. Plast Reconstr Surg. 2015;136(3):474-483. doi:10.1097/PRS.0000000000001498
- ^ Campisi, C. C., Ryan, M., Boccardo, F., & Campisi, C. (Accepted/In press). Fibro-Lipo-Lymph-Aspiration With a Lymph Vessel Sparing Procedure to Treat Advanced Lymphedema After Multiple Lymphatic-Venous Anastomoses: The Complete Treatment Protocol. Annals of Plastic Surgery. https://doi.org/10.1097/SAP.0000000000000853
- ^ Habbema L. Safety of liposuction using exclusively tumescent local anesthesia in 3,240 consecutive cases. Dermatol Surg. 2009;35(11):1728-1735. doi:10.1111/j.1524-4725.2009.01284.x
- ^ Jump up to: a b c Stephan, PJ; Kenkel, JM (2010). "Updates and advances in liposuction". Aesthetic Surgery Journal. 30 (1): 83–97. doi:10.1177/1090820X10362728. PMID 20442081.
- ^ Paik, AM; Daniali, LN; Lee, ES; Hsia, HC (2014). "Local anesthetic use in tumescent liposuction: an American Society of Plastic Surgeons survey". Annals of Plastic Surgery. 74 (2): 145–151. doi:10.1097/SAP.0000000000000420. PMID 25590254.
- ^ Tierney, Emily P.; Kouba, David J.; Hanke, C. William (December 2011). "Safety of tumescent and laser-assisted liposuction: review of the literature". Journal of Drugs in Dermatology. 10 (12): 1363–9. PMID 22134559.
- ^ Draelos, Zoe (2011). Cosmetic Dermatology: Products and Procedures. John Wiley & Sons. p. Chapter 56. ISBN 9781444359510.
- ^ Fischer A.; Fischer G. (1977). "Revised Technique for Cellulite fat reduction in Riding Breeches deformity". Bulletin of the International Academy of Cosmetic Surgery. 2 (4): 40–43.
- ^ Schiffman, p. 3.
- ^ Jump up to: a b c d e f g h Bellini, E; Grieco, MP; Raposio, E (December 2017). "A journey through liposuction and liposculture: Review". Annals of Medicine and Surgery (2012). 24: 53–60. doi:10.1016/j.amsu.2017.10.024. PMC 5681335. PMID 29158895.
- ^ Glicenstein, J (1989). "L'affaire Dujarier" [Dujarier's case]. Annales de Chirurgie Plastique Esthétique (in French). 34 (3): 290–2. PMID 2473691.
- ^ Sterodimas, A; Boriani, F; Magarakis, E; Nicaretta, B; Pereira, LH; Illouz, YG (March 2012). "Thirtyfour years of liposuction: past, present and future". European Review for Medical and Pharmacological Sciences. 16 (3): 393–406. PMID 22530358.
- ^ Chia, CT; Neinstein, RM; Theodorou, SJ (January 2017). "Evidence-Based Medicine: Liposuction". Plastic and Reconstructive Surgery. 139 (1): 267e–274e. doi:10.1097/PRS.0000000000002859. PMID 28027260.
External links[]
| Wikimedia Commons has media related to Liposuction. |
- Abdominal surgical procedures
- Management of obesity
- Medical ultrasonography
- Plastic surgery
- Surgical removal procedures