Hashimoto's encephalopathy
| Hashimoto's encephalopathy | |
|---|---|
| Other names | Steroid-responsive encephalopathy associated with autoimmune thyroiditis (SREAT) |
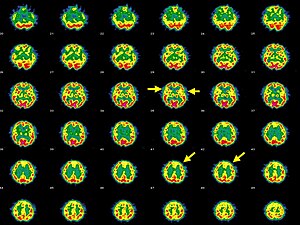 | |
| Brain SPECT transaxial images of a patient afflicted with Hashimoto's encephalopathy. | |
| Specialty | Neurology |
Hashimoto's encephalopathy, also known as steroid-responsive encephalopathy associated with autoimmune thyroiditis (SREAT), is a neurological condition characterized by encephalopathy, thyroid autoimmunity, and good clinical response to corticosteroids. It is associated with Hashimoto's thyroiditis, and was first described in 1966. It is sometimes referred to as a neuroendocrine disorder, although the condition's relationship to the endocrine system is widely disputed. It is recognized as a rare disease by the NIH Genetic and Rare Diseases Information Center.[1]
Up to 2005, almost 200 case reports of this disease were published. Between 1990 and 2000, 43 cases were published. Since that time, research has expanded and numerous cases are being reported by scientists around the world, suggesting that this rare condition is likely to have been significantly undiagnosed in the past. Over 100 scientific articles on Hashimoto's encephalopathy were published between 2000 and 2013.[2]
Signs and symptoms[]
The onset of symptoms tends to be fairly gradual and to occur over 1-12 years.[citation needed]
Symptoms of Hashimoto's encephalopathy may include:[citation needed]
- Personality changes
- Aggression
- Delusional behavior
- Concentration and memory problems
- Coma
- Disorientation
- Headaches
- Jerks in the muscles (myoclonus – 65% of cases)
- Lack of coordination (ataxia – 65% of cases)
- Partial paralysis on the right side
- Psychosis
- Seizures (60% of cases)
- Sleep abnormalities (55% of cases)
- Speech problems (transient aphasia – 80% of cases)
- Status epilepticus (20% of cases)
- Tremors (80% of cases)
Pathogenesis[]
The mechanism of pathogenesis is not known, but is thought to be an autoimmune disorder, similar to Hashimoto's thyroiditis, as its name suggests.[citation needed]
Consistent with this hypothesis, autoantibodies to alpha-enolase have been found to be associated with Hashimoto's encephalopathy.[3] Since enolase is the penultimate step in glycolysis, if it were inhibited (for example by being bound by autoantibodies), one would expect decreased energy production by each cell, leading to resulting atrophy of the affected organ.[citation needed]
This would occur most likely through each cell shrinking in size in response to the energy deficit (and/or in extreme situations from some cells dying via either apoptosis or necrosis, depending on location).[4] This may occur as a result of enough ATP not being available to maintain cellular functions - notably, failure of the Na/K ATPase, resulting in a loss of the gradient to drive the Na/Ca antiporter, which normally keeps Ca+
2 out of cells so it does not build to toxic levels that will rupture cell lysosomes leading to apoptosis. An additional feature of a low-energy state is failure to maintain axonal transport via dynein/kinesin ATPases, which in many diseases results in neuronal injury to both the brain and/or periphery.[5]
Pathology[]
Very little is known about the pathology of Hashimoto's encephalopathy. Post mortem studies of some individuals have shown lymphocytic vasculitis of venules and veins in the brain stem and a diffuse gliosis involving gray matter more than white matter.[citation needed]
As mentioned above, autoantibodies to alpha-enolase associated with Hashimoto's encephalopathy have thus far been the most hypothesized mechanism of injury.[3]
Diagnosis[]
Laboratory and radiological findings[]
- Increased liver enzyme levels (55% cases)
- Increased thyroid-stimulating hormone (55% cases)
- Increased erythrocyte sedimentation rate (25% cases)
Cerebrospinal fluid findings:[citation needed]
- Raised protein (25% cases)
- Negative for 14–3–3 protein
- May contain antithyroid antibodies
- Magnetic resonance imaging abnormalities consistent with encephalopathy (26% f cases)
- Single photon emission computed tomography shows focal and global hypoperfusion (75% of cases)
- Cerebral angiography is normal
Thyroid hormone abnormalities are common (>80% of cases):[citation needed]
- Subclinical hypothyroidism (35% of cases)
- Overt hypothyroidism (20% of cases)
- Hyperthyroidism (5% of cases)
- Euthyroid on levothyroxine (10% of cases)
- Euthyroid not on levothyroxine (20% of cases)
Thyroid antibodies – both antithyroid peroxidase antibodies (anti-TPO, antithyroid microsomal antibodies, anti-M) and antithyroglobulin antibodies (anti-Tg) – in the disease are elevated, but their levels do not correlate with the severity.[citation needed]
Electroencephalogram studies, while almost always abnormal (98% of cases), are usually not diagnostic. The most common findings are diffuse or generalized slowing or frontal intermittent rhythmic delta activity. Prominent triphasic waves, focal slowing, epileptiform abnormalities, and photoparoxysmal and photomyogenic responses may be seen.[6]
Definition[]
A relapsing encephalopathy occurs in association with Hashimoto's thyroiditis, with high titers of antithyroid antibodies. Clinically, the condition may present one or more symptoms. Onset is often gradual and may go unnoticed by the patient and close associates to the patients. Symptoms sometimes resolve themselves within days to weeks, leaving a patient undiagnosed. For many other patients, the condition may result in ongoing problems with a variety of manifestations, often confusing clinicians due to the diffuse nature of symptoms.[citation needed]
Differential diagnosis[]
- Alzheimer's disease
- Cerebrovascular accidents (stroke)
- Creutzfeldt–Jakob disease
- Epilepsy
- Migraine (including basilar, hemiplegic, and retinal types)
- Other forms of autoimmune encephalitis, including forms of limbic encephalitis such as anti-NMDA receptor encephalitis
- Schizophrenia
- Spontaneous cerebrospinal fluid leak
- Viral encephalitis
- Transient ischemic attack
Treatment[]
Because most patients respond to corticosteroids or immunosuppressant treatment, this condition is now also referred to as steroid-responsive encephalopathy.[citation needed]
Initial treatment is usually with oral prednisone (50–150 mg/day) or high-dose intravenous methylprednisolone (1 g/day) for 3–7 days. Thyroid hormone treatment is also included if required.Failure of some patients to respond to this first-line treatment has produced a variety of alternative treatments, including azathioprine, cyclophosphamide, chloroquine, methotrexate, periodic intravenous immunoglobulin, and plasma exchange. No controlled trials have been conducted, so the optimal treatment is not known.[citation needed]
Seizures, if present, are controlled with typical antiepileptic agents.[citation needed]
Prognosis[]
Duration of treatment is usually between 2 and 25 years. Earlier reports suggested that 90% of cases stay in remission after discontinuation of treatment, but this is at odds with more recent studies, which suggest that relapse commonly occurs after initial high-dose steroid treatment.[7][8] Left untreated, this condition can result in coma and death.
Epidemiology[]
The prevalence has been estimated to be 2.1/100,000[9] with a male-to-female ratio of 1:4. The mean age of onset is 44 with 20% of cases presenting before the age of 18 years. Most reported cases occur during the patient's fifth decade of life.[citation needed]
History[]
The first case of HE was described by Brain et al. in 1966.[10] The patient was a 48-year-old man with hypothyroidism, multiple episodes of encephalopathy, stroke-like symptoms, and Hashimoto's thyroiditis confirmed by elevated antithyroid antibodies.
Alternative names[]
- Steroid-responsive encephalopathy associated with autoimmune thyroiditis, SREAT
- Nonvasculitic autoimmune meningoencephalitis, NAIM
- Encephalopathy associated with autoimmune thyroid disease, EAATD
References[]
- ^ "Hashimoto's encephalitis - Disease - Overview". Genetic and Rare Diseases Information Center (GARD).
- ^ "Scientific Research/Articles – Articles Published in 2014". hesaonline.org. Archived from the original on 2013-07-08.
- ^ Jump up to: a b Fujii A, Yoneda M, Ito T, Yamamura O, Satomi S, Higa H, Kimura A, Suzuki M, Yamashita M, Yuasa T, Suzuki H, Kuriyama M (May 2005). "Autoantibodies against the amino terminal of alpha-enolase are a useful diagnostic marker of Hashimoto's encephalopathy". J. Neuroimmunol. 162 (1–2): 130–6. doi:10.1016/j.jneuroim.2005.02.004. PMID 15833368. S2CID 43249019.
- ^ Shigeomi Shimizu2, Yutaka Eguchi, Wataru Kamiike, Yuko Itoh, Jun-ichi Hasegawa, Kazuo Yamabe, Yoshinori Otsuki, Hikaru Matsuda, and Yoshihide Tsujimoto The First Department of Surgery. Department of Medical Genetics. BiomedicalResearch Center. Osaka University Medical School, 2-2 Yatnadfioka, Sunti 56.5. Japan, and Depannient of Anatomy and Biology. Osaka Medical College. Japan.| url=http://cancerres.aacrjournals.org/content/56/9/2161.full.pdf
- ^ Ihejirika DF. PASS Program Course Notes: USMLE Preparation. Lulu.com; 2014.
- ^ Li, Jie; Li, Fengzhen (2019-05-08). "Hashimoto's Encephalopathy and Seizure Disorders". Frontiers in Neurology. 10: 440. doi:10.3389/fneur.2019.00440. ISSN 1664-2295. PMC 6517482. PMID 31133960.
- ^ Castillo P, Woodruff B, Caselli R, et al. (February 2006). "Steroid-responsive encephalopathy associated with autoimmune thyroiditis". Archives of Neurology. 63 (2): 197–202. doi:10.1001/archneur.63.2.197. PMID 16476807.
- ^ Flanagan EP, McKeon A, Lennon VA, et al. (October 2010). "Autoimmune dementia: clinical course and predictors of immunotherapy response". Mayo Clinic Proceedings. 85 (10): 881–97. doi:10.4065/mcp.2010.0326. PMC 2947960. PMID 20884824.
- ^ Ferracci F, Bertiato G, Moretto G (February 2004). "Hashimoto's encephalopathy: epidemiologic data and pathogenetic considerations". Journal of the Neurological Sciences. 217 (2): 165–8. doi:10.1016/j.jns.2003.09.007. PMID 14706219. S2CID 19827218.
- ^ Brain L, Jellinek EH, Ball K (September 1966). "Hashimoto's disease and encephalopathy". The Lancet. 2 (7462): 512–4. doi:10.1016/S0140-6736(66)92876-5. PMID 4161638.
Further reading[]
- Hashimoto's Encephalopathy SREAT Alliance (2013). Understanding Hashimoto's Encephalopathy: A Guide for Patients, Families, and Caregivers, Featuring Stories of HE Patients from Around the World. North Charleston, SC: CreateSpace Independent Publishing Platform. ISBN 9781484883099. OCLC 890816771.
- Schiess N, Pardo CA (October 2008). "Hashimoto's encephalopathy". Annals of the New York Academy of Sciences. 1142 (1): 254–65. Bibcode:2008NYASA1142..254S. doi:10.1196/annals.1444.018. PMID 18990131. S2CID 1312798.
- Taylor SE, Garalda ME, Tudor-Williams G, Martinez-Alier N (February 2003). "An organic cause of neuropsychiatric illness in adolescence". The Lancet. 361 (9357): 572. doi:10.1016/S0140-6736(03)12517-2. PMID 12598143. S2CID 35053683.
| Classification |
|---|
- Autoimmune diseases
- Brain disorders
- Neuroendocrinology
- Steroid-responsive inflammatory conditions
