Salivary gland disease
| Salivary gland disease | |
|---|---|
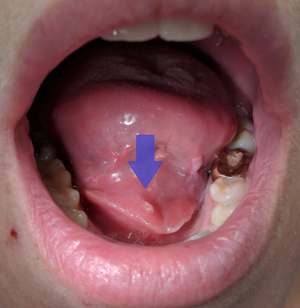 | |
| Blockage of the submandibular gland by a stone with subsequent infection. Arrow marks pus coming out of the opening of the submandibular gland | |
| Specialty | Gastroenterology, oral and maxillofacial surgery |
Salivary gland diseases (SGD) are multiple and varied in cause.[1]
There are three paired major salivary glands in humans – (the parotid glands, the submandibular glands, and the sublingual glands), and about 800-1000 minor salivary glands in the mucosa of the mouth. The parotid gland is located in front of the ear, and it secretes its mostly serous saliva via the parotid duct (Stenson duct) into the mouth, usually opening roughly opposite the maxillary second molar. The submandibular gland is located medial to the angle of the mandible, and it drains its mixture of serous and mucous saliva via the submandibular duct (Wharton duct) into the mouth, usually opening in a punctum located in the floor of mouth. The sublingual gland is located below the tongue, on the floor of the mouth. It drains its mostly mucous saliva into the mouth via about 8-20 ducts which open along the plica sublingualis (a fold of tissue under the tongue).[2]
The function of the salivary glands is to secrete saliva, which has a lubricating function, which protects the oral mucosa of the mouth during eating and speaking.[2] Saliva also contains digestive enzymes (e.g. salivary amylase) and has antimicrobial action and acts as a buffer.[3] Salivary gland dysfunction occurs when salivary rates are reduced and this can result in xerostomia (dry mouth).[4]
Various examples of disorders affecting the salivary glands are listed below. Some are more common than others, and they are considered according to a surgical sieve, but this list is not exhaustive. Sialadenitis is inflammation of a salivary gland, usually caused by infections, although there are other less common causes of inflammation such as irradiation, allergic reactions or trauma.[5]
Congenital[]

Congenital disorders of the salivary glands are rare,[5] but may include:
- Aplasia
- Atresia
- Ectopic salivary gland tissue
- Stafne defect - an uncommon condition which some consider to be an anatomic variant rather than a true disease. It is thought to be created by an ectopic portion of salivary gland tissue which causes the bone of the mandible to remodel around the tissue, creating an apparent cyst like radiolucent area on radiographs. Classically, this lesion is discovered as a chance finding,[6] since it causes no symptoms. It appears below the inferior alveolar nerve canal in the posterior region of the mandible.
Acquired[]
Dysfunction[]
Salivary gland dysfunction affects the flow, amount, or quality of saliva produced. A reduced salivation is termed hyposalivation. Hyposalivation often results in a dry mouth condition called xerostomia, and this can cause tooth decay due to the loss of the protective properties of saliva. In addition, The results of a study [7] have suggested that hyposalivation could lead to acute respiratory infection. There are two potential reasons for increasing the incidence rate of this infection. First, reduced saliva secretion may impair the oral and airway mucosal surface as a physical barrier, which consequently enhances the adhesion and colonization of viruses. Second, this reduction may also impair the secretion of antimicrobial proteins and peptides.[7] Considering presence of many proteins and peptides with established antiviral properties in saliva, some of which can potentially inhibit virus replication especially coronavirus, it gives the impression that the protective effect of these salivary proteins against the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) might be the same.[8] Therefore, hyposalivation could be a potential risk factor for acute respiratory infection. It may expose patients at high risk of getting coronavirus disease (COVID-19). However, further investigations are crucial to prove this hypothesis.[8]
Hypersalivation is the overproduction of saliva and has many causes.[9][10]
Vascular[]
- Necrotizing sialometaplasia—a lesion that usually arises from a minor salivary gland on the palate. It is thought to be due to vascular infarction of the salivary gland lobules. It is often mistaken for oral cancer, but the lesion is not neoplastic.[2]
Infective[]
Infections involving the salivary glands can be viral or bacterial (or rarely fungal).
- Mumps is the most common viral sialadenitis. It usually occurs in children, and there is preauricular pain (pain felt in front of the ear), swelling of the parotid, fever, chills, and headaches.[2]
- Bacterial sialadenitis is usually caused by ascending organisms from the oral cavity. Risk factors include reduced salivary flow rate.
- Human immunodeficiency virus-associated salivary gland disease (HIV-SGD).[1]
Traumatic[]

- Mucocele — these are common and are caused by rupture of a salivary gland duct and mucin spillage into the surrounding tissues. Usually, they are caused by trauma. Classically, a mucocele is bluish and fluctuant, and most commonly occurs on the lower lip.[11]
- Ranula — the name used when a mucocele occurs in the floor of the mouth (underneath the tongue). Ranulas may grow to a larger size than mucoceles at other sites, and they are usually associated with the sublingual gland, although less commonly they may also arise from the submandibular gland or a minor salivary gland.[11] Uncommonly, a ranula may descend into the neck rather than the mouth (plunging ranula). If small, the ranula may be left alone, but if larger and causing symptoms, excision of the sublingual gland may be indicated.
- Nicotinic stomatitis — the hard palate is whitened by hyperkeratosis caused by the heat from tobacco use or hot liquid consumption. This irritation also causes inflammation of the duct openings of the minor salivary glands of the palate, and they become dilated. This manifests as red patches or spots on a white background.[12]
Autoimmune[]
- Sjögren's syndrome
- Graft-versus-host disease
Inflammatory[]
- Post-irradiation sialadenitis
- Sarcoidosis—there may be parotitis alone or uveoparotitis (inflammation of both the parotid and the uvea of the eyes), which occurs in Heerfordt's syndrome.
- Cheilitis glandularis—This is inflammation of the minor salivary glands, usually in the lower lip, eversion and swelling of the lip.[11]
- Chronic sclerosing sialadenitis is a salivary gland manifestation of IgG4-related disease.[13][14]
Neurological[]
Neoplastic[]
- Salivary gland neoplasm
Diverticulum[]
A salivary diverticulum (plural diverticuli) is a small pouch or out-pocketing of the duct system of a major salivary gland.[15] Such diverticuli typically cause pooling of saliva and recurrent sialadenitis,[16] especially parotitis.[17] A diverticulum may also cause a sialolith to form.[18][19] The condition can be diagnosed by sialography.[16] Affected individuals may "milk" the salivary gland to encourage flow of saliva through the duct.[16]
Unknown[]
- Sialolithiasis - although several possibly coexisting factors have been suggested to be involved in the formation of salivary stones, including altered acidity of saliva, reduced salivary flow rate, abnormal calcium metabolism and abnormalities in the sphincter mechanism of the duct opening, the exact cause in many cases is unknown.
- Sialadenosis (sialosis) is an uncommon, non-inflammatory, non-neoplastic, recurrent swelling of the salivary glands. The cause is hypothesized to be abnormalities of neurosecretory control. It may be associated with alcoholism.[5][20][21]
References[]
- ^ a b Jeffers, L; Webster-Cyriaque, JY (April 2011). "Viruses and salivary gland disease (SGD): lessons from HIV SGD". Advances in Dental Research. 23 (1): 79–83. doi:10.1177/0022034510396882. PMC 3144046. PMID 21441486.
- ^ a b c d Hupp JR, Ellis E, Tucker MR (2008). Contemporary oral and maxillofacial surgery (5th ed.). St. Louis, Mo.: Mosby Elsevier. pp. 397–419. ISBN 9780323049030.
- ^ Brown, T. Rapid Review Physiology. Mosby Elsevier. p. 235.
- ^ "Diseases of the Salivary Glands". The Lecturio Medical Concept Library. Retrieved 12 July 2021.
- ^ a b c Soames JV, Southam JC, JV (1999). Oral pathology (3rd ed.). Oxford: Oxford Univ. Press. pp. 247–265. ISBN 978-0192628947.
- ^ Wray D, Stenhouse D, Lee D, Clark AJ (2003). Textbook of general and oral surgery. Edinburgh [etc.]: Churchill Livingstone. pp. 236–237. ISBN 978-0443070839.
- ^ a b Iwabuchi, Hiroshi; Fujibayashi, Takashi; Yamane, Gen-yuki; Imai, Hirohisa; Nakao, Hiroyuki (2012). "Relationship between Hyposalivation and Acute Respiratory Infection in Dental Outpatients". Gerontology. 58 (3): 205–211. doi:10.1159/000333147. ISSN 1423-0003. PMID 22104982.
- ^ a b Farshidfar, Nima; Hamedani, Shahram (2020-04-29). "Hyposalivation as a potential risk for SARS‐CoV‐2 infection: Inhibitory role of saliva". Oral Diseases: odi.13375. doi:10.1111/odi.13375. ISSN 1354-523X. PMC 7267261. PMID 32348636.
- ^ McGeachan AJ, Mcdermott CJ (10 February 2017). "Management of oral secretions in neurological disease". Practical Neurology (Review). Association of British Neurologists. 17 (2): 96–103. doi:10.1136/practneurol-2016-001515. PMID 28188210 – via BMJ Journals.
- ^ Miranda-Rius J, Brunet-Llobet L, Lahor-Soler E, Farré M (22 September 2015). "Salivary Secretory Disorders, Inducing Drugs, and Clinical Management". International Journal of Medical Sciences (Review). Ivyspring. 12 (10): 811–824. doi:10.7150/ijms.12912. PMC 4615242. PMID 26516310.
- ^ a b c Neville BW, Damm DD, Allen CA, Bouquot JE (2002). Oral & maxillofacial pathology (2nd ed.). Philadelphia: W.B. Saunders. pp. 389–430. ISBN 978-0721690032.
- ^ Illustrated Dental Embryology, Histology, and Anatomy, Bath-Balogh and Fehrenbach, Elsevier, 2011, page 137
- ^ John H. Stone; Arezou Khosroshahi; Vikram Deshpande; et al. (October 2012). "Recommendations for the nomenclature of IgG4-related disease and its individual organ system manifestations". Arthritis & Rheumatism. 64 (10): 3061–3067. doi:10.1002/art.34593. PMC 5963880. PMID 22736240.
- ^ Aly, Fatima (2011-10-07). "Salivary glands: Inflammation: Sialadenitis". Pathology Outlines. Retrieved 2013-12-05.
- ^ Ghom AG; Ghom SA (1 July 2014). Textbook of Oral Medicine. JP Medical Ltd. p. 606. ISBN 978-93-5152-303-1.
- ^ a b c Glick M (1 September 2014). Burket's oral medicine (12th ed.). coco. p. 233. ISBN 978-1-60795-188-9.
- ^ Chaudhary M; Chaudhary SD (1 April 2012). Essentials of Pediatric Oral Pathology. JP Medical Ltd. p. 304. ISBN 978-93-5025-374-8.
- ^ Afanas'ev, VV; Abdusalamov, MR (2004). "[Diverticulum of the submandibular salivary gland ducts]". Stomatologiia. 83 (5): 31–3. PMID 15477837.
- ^ Ligtenberg A; Veerman E (31 May 2014). Saliva: Secretion and Functions. Karger Medical and Scientific Publishers. p. 141. ISBN 978-3-318-02596-5.
- ^ Pape, SA; MacLeod, RI; McLean, NR; Soames, JV (September 1995). "Sialadenosis of the salivary glands". British Journal of Plastic Surgery. 48 (6): 419–22. doi:10.1016/s0007-1226(95)90233-3. PMID 7551515.
- ^ Mandel, L; Hamele-Bena, D (October 1997). "Alcoholic parotid sialadenosis". Journal of the American Dental Association. 128 (10): 1411–5. doi:10.14219/jada.archive.1997.0060. PMID 9332142.
External links[]
| Wikimedia Commons has media related to Diseases and disorders of salivary glands. |
- Salivary gland pathology